Fungal Acne: An In-Depth Exploration
What is Fungal Acne?
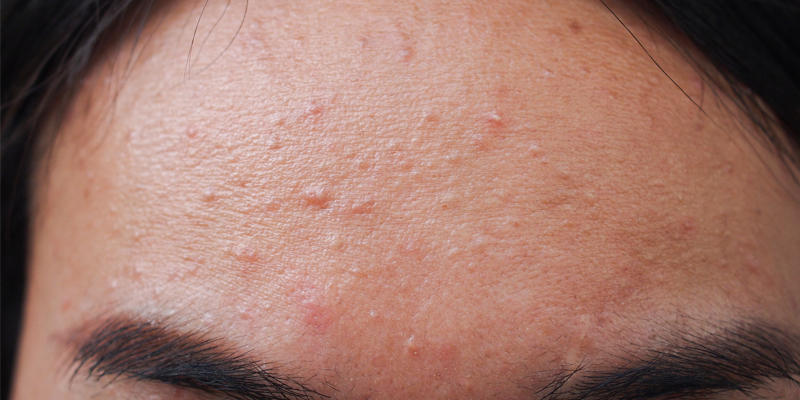
Fungal acne, scientifically known as Malassezia folliculitis, is a skin condition often misinterpreted as traditional acne. It emerges as a consequence of an overgrowth of a yeast-like fungus called Malassezia, naturally residing on the skin's surface. When Malassezia proliferates within hair follicles, it gives rise to small, itchy, acne-like bumps. These tiny bumps usually display a uniform size, often sporting a reddish or skin-colored hue and sometimes congregating in clusters. Unlike regular acne, fungal acne doesn't lead to blackheads or whiteheads and is not accompanied by pain or tenderness.
Fungal acne frequently appears in regions with a high density of oil glands, such as the forehead, chest, and back. Factors like humidity, perspiration, and the use of oily or comedogenic (pore-clogging) skincare products can exacerbate this condition.
Distinguishing Fungal Acne from Regular Acne
Fungal acne and regular acne (also known as acne vulgaris) have different causes and characteristics. Here are the key differences between the two:
Fungal Acne:
- Cause: Fungal acne arises from an overgrowth of the yeast-like fungus Malassezia, naturally present on the skin. When Malassezia proliferates in hair follicles, it results in small, itchy, acne-like bumps.
- Appearance: Fungal acne typically presents as small, uniform papules or pustules, often with a reddish or skin-colored appearance. These lesions may itch, but they don't produce blackheads or whiteheads. Fungal acne commonly emerges in areas abundant in oil glands, like the forehead, chest, and back, but can affect other body areas.
- Itching: Itchiness is a common symptom of fungal acne.
Regular Acne (Acne Vulgaris):
- Cause: Regular acne, or acne vulgaris, primarily stems from various factors, including excess oil production, clogged hair follicles, the presence of bacteria (Propionibacterium acnes), and inflammation. It leads to various types of lesions, including blackheads, whiteheads, pustules, and cysts.
- Appearance: Regular acne can manifest as a combination of lesion types, including blackheads (open comedones), whiteheads (closed comedones), pustules, papules, nodules, and cysts. It often involves a mixture of lesion types, with varying appearances. Regular acne can appear on the face, neck, chest, back, shoulders, and sometimes other body regions, and is not restricted to areas with high oil gland density. Itching is not a characteristic symptom of regular acne, although some individuals with acne may experience minor discomfort or irritation.
Who is Prone to Fungal Acne?
Fungal acne can affect individuals across diverse age groups and backgrounds. Nonetheless, several factors may increase the likelihood of developing this condition:
- Oily Skin: Individuals with naturally oily skin are more susceptible to fungal acne, as the surplus oil provides an ideal environment for the Malassezia fungus to flourish.
- Teens and Young Adults: Fungal acne can be more prevalent among teenagers and young adults. This age group often experiences increased oil production due to hormonal changes, contributing to fungal acne.
- Suppressed Immune Systems: Individuals with weakened immune systems, such as those with HIV/AIDS, undergoing chemotherapy, or taking immunosuppressive medications, may be more vulnerable to fungal infections, including fungal acne.
- Pregnant Women: Hormonal changes during pregnancy can elevate oil production, occasionally increasing the risk of fungal acne.
- Hot and Humid Environments: Fungal acne thrives in warm, humid conditions. Consequently, individuals residing in high-temperature, high-humidity climates may face a greater susceptibility to this condition.
- Frequent Sweating: Engaging in activities that induce frequent perspiration, such as athletics or physically demanding occupations, may elevate the risk of fungal acne due to the conducive environment for fungal growth.
- Antibiotic Usage: Extended antibiotic use can disturb the skin's natural microorganism balance, possibly resulting in Malassezia overgrowth and an increased risk of fungal acne.
- High-Potency Topical Steroids: Prolonged usage of high-potency topical steroids can alter the skin's environment, potentially contributing to fungal acne.
- History of Skin Conditions: Individuals with a history of skin conditions like eczema or seborrheic dermatitis may be more susceptible to fungal acne, as these conditions are associated with increased colonization of Malassezia.
It's essential to acknowledge that while these factors may heighten the risk of developing fungal acne, the condition can affect anyone, regardless of age or background.
Triggers of Fungal Acne
Understanding the factors that can trigger or exacerbate fungal acne is crucial for managing and preventing its recurrence. Here are some common triggers to be aware of:
- Humidity and Sweat: Fungal acne thrives in warm, humid environments. Excessive sweating can create an ideal breeding ground for the Malassezia fungus. Be sure to shower and change into clean, dry clothes after sweating to prevent its development.
- Oily Skin: Excessive oil production on your skin can provide a food source for the Malassezia fungus. If you have naturally oily skin, it's essential to choose skincare products that are non-comedogenic and oil-free.
- Hormonal Changes: Hormonal fluctuations can trigger or worsen fungal acne. This is especially common in teenagers, pregnant women, and those with certain medical conditions. Hormonal therapies may be necessary for management.
- Diet: While diet isn't a primary cause of fungal acne, consuming a high-sugar or high-glycemic diet may encourage fungal overgrowth. Consider adopting a balanced diet to support skin health.
- Prolonged Antibiotic Use: Antibiotics can disrupt the natural balance of microorganisms on your skin. Long-term use of antibiotics can potentially contribute to fungal acne by allowing the Malassezia fungus to proliferate.
- Comedogenic Products: Using skincare and makeup products that clog pores (comedogenic products) can exacerbate fungal acne. Check product labels for non-comedogenic options.
- Tight Clothing: Wearing tight, non-breathable clothing can trap moisture and sweat against your skin, creating conditions favorable for fungal acne. Choose loose-fitting, breathable fabrics whenever possible.
- Prolonged Exposure to High Humidity or Heat: Living in a humid climate or frequently being exposed to high heat and humidity can increase your risk of fungal acne. Consider using cooling and drying products or staying in climate-controlled environments.
- Over-cleansing: While maintaining good hygiene is crucial, over-cleansing your skin can strip it of natural oils, potentially leading to increased oil production. Stick to a gentle cleansing routine.
By identifying and managing these triggers, you can significantly reduce the risk of fungal acne and improve your overall skin health.
Recognizing the Symptoms of Fungal Acne
- Fungal acne manifests with distinct symptoms that differentiate it from traditional acne. The common symptoms of fungal acne include:
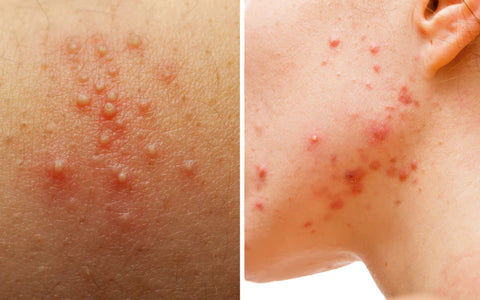
- Uniform Appearance: Unlike regular acne, which may vary in size and shape, fungal acne typically appears as small, uniform papules or pustules. They are often the same size and have a reddish or skin-colored appearance.
- Itching: One of the key indicators of fungal acne is itching. If you notice that your acne lesions are particularly itchy, it might be a sign that it's fungal.
- Clusters of Bumps: Fungal acne tends to cluster in groups or lines along the skin, often in areas with a high concentration of oil glands, like the forehead, chest, and back.
- No Blackheads or Whiteheads: Fungal acne doesn't produce blackheads or whiteheads, which are common in traditional acne. If you're not seeing these types of lesions, it could be an indication of fungal acne.
- Persistence: Fungal acne can be persistent and may not respond well to traditional acne treatments like benzoyl peroxide or salicylic acid.
- Worsening with Sweat or Heat: Fungal acne can exacerbate with sweat and heat. If you notice that your breakouts tend to worsen after exercise or in hot, humid conditions, it could be a sign of fungal acne.
- Absence of Pain: Unlike cystic acne, which can be painful, fungal acne is typically not associated with pain or tenderness.
How is Fungal Acne Diagnosed?
Diagnosing fungal acne typically involves a combination of clinical evaluation and, in some cases, laboratory tests. Here are the steps involved in the diagnosis:
- Clinical Evaluation: A dermatologist or healthcare provider will perform a thorough clinical evaluation of your skin. They will examine the appearance and distribution of your skin lesions. Key characteristics that can indicate fungal acne include small, uniform papules or pustules, itching, and clustering of bumps. The absence of blackheads and whiteheads is also a common feature.
- Medical History: Your healthcare provider may ask about your medical history, including any recent changes in skincare products, medications, or lifestyle factors that may be contributing to your skin condition. They will also inquire about your symptoms, such as itching, and any factors that exacerbate your skin issues.
- Wood's Lamp Examination: In some cases, a Wood's lamp, which emits ultraviolet (UV) light, may be used to examine the skin. Under this light, Malassezia fluoresces, allowing the healthcare provider to visually confirm the presence of the fungus. However, not all cases of fungal acne are diagnosed through this method.
- Skin Swab or Biopsy: In more challenging or uncertain cases, a skin swab or biopsy may be performed. This involves taking a small sample of the affected skin for laboratory analysis. The sample can be examined under a microscope to confirm the presence of Malassezia or to rule out other skin conditions.
How to Treat Fungal Acne Naturally
Natural remedies, often derived from plant-based or organic sources, can offer a more holistic and gentle alternative for those seeking to address fungal acne without the potential side effects of pharmaceutical options.
Here are some natural approaches to consider:
- Tea Tree Oil: Tea tree oil is a natural antifungal and antibacterial agent. You can dilute tea tree oil with carrier oil (like coconut or jojoba oil) and apply it to the affected areas. Be cautious with tea tree oil, as it can be harsh on the skin if not properly diluted. Perform a patch test first to check for sensitivity.
- Apple Cider Vinegar: Apple cider vinegar has antifungal properties and may help control Malassezia growth. Mix one part apple cider vinegar with one part water, and use a cotton ball to apply it to the affected areas. Rinse it off after a few minutes.
- Aloe Vera: Aloe vera gel has soothing and anti-inflammatory properties. Apply a thin layer of pure aloe vera gel to the affected areas to help calm inflammation and discomfort.
- Coconut Oil: Some individuals find that using coconut oil as a moisturizer can be helpful. Coconut oil has natural antifungal properties, but it can be comedogenic for some people, so use it sparingly.
- Gentle Cleansing: Use a gentle, pH-balanced cleanser to keep the affected areas clean. Avoid harsh or abrasive cleansers, as they can irritate the skin.
- Probiotics: Consuming probiotics through foods like yogurt or dietary supplements may help support a healthy balance of microorganisms on the skin. A balanced microbiome can potentially discourage fungal overgrowth.
- Dietary Adjustments: Reducing your intake of sugary and high-glycemic foods may help manage fungal overgrowth. A balanced diet can support skin health.
- Stress Reduction: Stress can exacerbate skin conditions. Engaging in stress-reduction techniques like meditation, yoga, or exercise may help keep stress levels in check.
- Stay Dry and Cool: Avoid tight clothing and stay in climate-controlled environments to minimize sweating and humidity, which can worsen fungal acne.
Managing and Preventing Fungal Acne at Home
While consulting a dermatologist is an option for effective treatment of fungal acne, there are steps you can take at home to manage and prevent its recurrence:
- Use Antifungal Body Washes: Incorporate antifungal body washes or shampoos with active ingredients like ketoconazole or selenium sulfide into your daily shower routine. Pay special attention to areas prone to fungal acne, such as your chest and back.
- Gentle Cleansing: Avoid harsh, abrasive cleansers that can disrupt your skin's natural barrier. Opt for gentle, pH-balanced cleansers to maintain skin health without over-drying.
- Non-comedogenic Products: Choose skincare and makeup products labeled as "non-comedogenic." These won't clog your pores, reducing the risk of fungal acne.
- Keep Skin Dry: After sweating, make sure to shower promptly and change into clean, dry clothes. This helps prevent the buildup of sweat and moisture that can exacerbate fungal acne.
- Breathable Fabrics: Opt for loose-fitting, breathable clothing made from natural fibers like cotton. Avoid tight, synthetic materials that can trap moisture against your skin.
- Balanced Diet: A well-balanced diet rich in fruits, vegetables, and whole grains can support overall skin health. Minimize sugary and high-glycemic foods, which may contribute to fungal overgrowth.
- Reduce Stress: Stress can worsen skin conditions, including fungal acne. Practice stress-reduction techniques like meditation, yoga, or exercise to help keep stress levels in check.
- Avoid Over-Treatment: Using too many products or over-treating your skin can sometimes worsen fungal acne. Stick to a simple skincare routine and avoid excessive use of harsh products.
- Regularly Wash Bedding: Regularly wash your bedding, especially pillowcases, to prevent the accumulation of oils and sweat that can lead to fungal acne.
- Avoid Hot and Humid Environments: When possible, stay in climate-controlled environments to reduce exposure to high heat and humidity, which can exacerbate fungal acne.
- Monitor Your Skin: Keep a close eye on your skin for any signs of fungal acne or its recurrence. Early detection can lead to more effective treatment.
In conclusion, while fungal acne can be challenging, with proper care, it is manageable and preventable. By understanding the signs, triggers, and home care strategies, you can take control of your skin health and enjoy a clearer, more comfortable complexion.
What to Do Next? Try Averr Aglow’s Clear Skin Kit
Tired of feeling lost and confused about what you should do to get clear, smooth skin? Order the Clear Skin Kit.
The Clear Skin Kit contains products specially crafted with the perfect blend of natural ingredients that help soothe and calm red, irritated skin while also clearing up breakouts. If you struggle with sensitive acne/breakout-prone skin, hormonal acne, cystic acne, or rosacea, then you’ll be happy you found this complete routine.
Please understand, that results may vary, we’re not selling you a miracle product and would never try to position or state that you will get a true result in only a few days. In our clinical trials, most users found the most results at the 30-day and then the 56-day mark by sticking with our routine.
What is Averr Aglow®?
Averr means Truth. We have pioneered a revolutionary no-rinse cleansing routine specifically tailored to address problematic skin issues.
Hi, I’m Camille, founder of Averr Aglow, and I help adult women who are battling breakouts and acne get clear skin results like they have never seen before, even if nothing has worked for them in the past.
After battling breakouts for over 16 years, trying every skincare product under the sun, and visiting countless professionals like dermatologists, nutritionists, and hormonal doctors, I finally learned why nothing seemed to work on clearing up my skin, what truly causes breakouts and acne, and EXACTLY what to do to get clear skin results – and I want to help you do the same.
Let me help you! Read my full testimonial here.






